Cannabis has been used for centuries, with evidence suggesting its medicinal use as early as 400 B.C. Interest in Cannabis’ potential medical benefits has garnered more attention since the discovery in the early 1990s of the effect of Cannabis on the body’s endocannabinoid system. Since the legalization of marijuana in Canada and deregulation and legalization in many parts of the U.S., there has been a growing body of research into Cannabis’ therapeutic effects.
What are the true health benefits of Cannabis and its constituents? What are its physiological effects and potential medical benefits? How have the purported medical effects been proven?
History of Cannabis use
Archaeological findings indicate that Cannabis was cultivated for its fibers to use in textiles, rope and paper thousands of years ago. The oldest evidence of Cannabis medicinal use dates back about 2,700 years ago. The discovery was made from the excavation of an ancient tomb in Northern China. Phytochemical analysis of vegetative manner found in a leather basket and wooden brazier, used for burning material, was identified as Cannabis sativa L.
In the 1940s, cannabidiol (CBD) and tetrahydrocannabinol (THC) were among the first cannabinoids to be extracted from the Cannabis plant. Twenty years later, CBD and THC were both chemically synthesized in a laboratory setting. CBD and THC are considered the ‘major’ cannabinoids given that they are the most abundant in the plant and, therefore, the most studied of the cannabinoid class of compounds. More than 100 other individual cannabinoid compounds have since been identified. These ‘rare’ cannabinoids account for less than 1% of the plant in total, making them much more difficult to extract and study. As such, research into rare cannabinoids is limited.
Cannabis and the endocannabinoid system
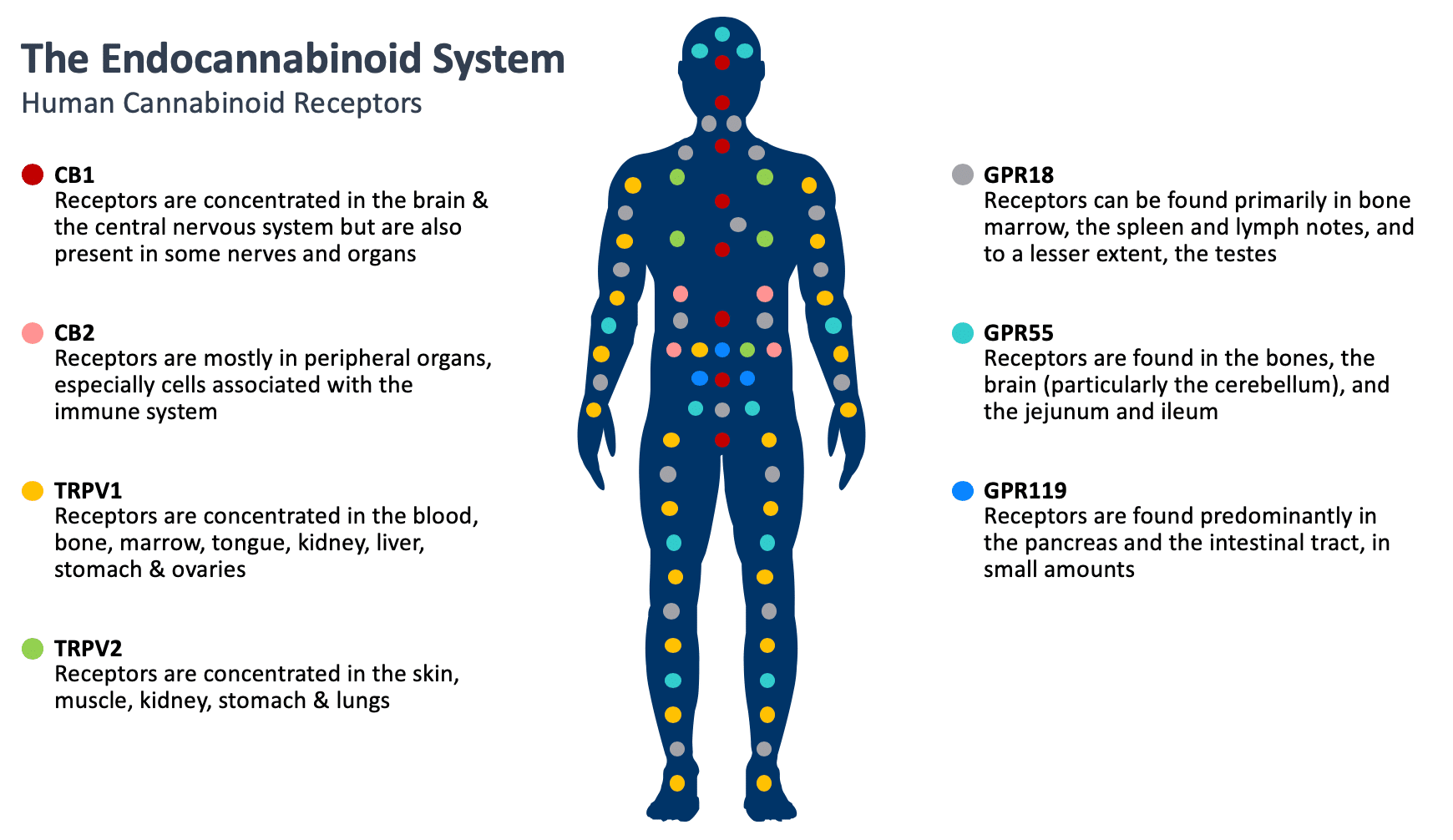
In the early 1990s, two cannabinoid receptors were discovered in humans, specifically endocannabinoid receptor 1 (CB1), which is more significant to the central nervous system, and endocannabinoid receptor 2 (CB2), which is associated with the immune system. Cannabinoid receptors are found throughout the body and are involved in many different functions, such as pain perception, memory, immune function and sleep. Cannabinoids act as messengers that bind to cannabinoid receptors, as well as other receptors, signaling the endocannabinoid and other body systems into action. The relevance of the endocannabinoid system on many important physiological processes has made cannabinoids an important target to potentially treat a number of diseases and symptoms.
More than 100 cannabinoids and over 400 other active compounds, called terpenes, are found in the Cannabis plant. Each cannabinoid has a specific structure that confers unique physiological properties in humans. Evidence demonstrates that even a slight difference in the structure of these compounds can result in profound differences in biological activity, safety and potential therapeutic effect in the human body.
Access to cannabinoids
There are two main ways to access cannabinoids – extract them from the Cannabis plant or manufacture them synthetically. The Cannabis plant may be cultivated and processed for use as a smokable product or as an extract. It can be challenging to access highly pure individual cannabinoids through the plant-grow-harvest-extract-purify method. Manufacturing cannabinoids synthetically, whereby cannabinoids are produced using sophisticated pharmaceutical-grade manufacturing processes, generates highly pure, individual cannabinoids. This level of purity is important for specific uses such as pharmaceutical use as a potential treatment.
Research into medical benefits of Cannabis
Each cannabinoid has a specific structure that confers unique physiological properties in humans. Slight difference in the structure of these compounds can result in profound differences in biological activity, safety and potential therapeutic effect in the human body.
Prohibition of Cannabis has limited the amount of scientific and clinical research to date, but with expanding legalization in various regions, the importance of research is emerging and we are starting to gain scientific evidence of its physiological effects and potential uses. Most of the Cannabis research to date has focused on CBD and THC, the most prevalent cannabinoids in the plant. This growing body of research has suggested potential therapeutic benefits in a wide variety of conditions. According to the book “The Health Benefits of Cannabis and Cannabinoids: The Current State of Evidence and Recommendations for Research” the most common conditions for which medical Cannabis is used are multiple sclerosis-related spasticity, nausea, post-traumatic stress disorder, cachexia, epilepsy, and treatment of symptoms, including pain, related to cancer, glaucoma, HIV/AIDS and degenerative neurological conditions.
Much of the research to date has been observational and has not been conducted through the clinical trial process. A clinical trial requires several parameters of qualitative and quantitative evidence to prove its safety and effectiveness before it is approved for consumers. Without clinical trial evidence, it’s much too early to make claims of Cannabis’ true therapeutic benefits and safety.
What is the difference between pharmaceutical-grade and medicinal Cannabis?
Pharmaceutical and medicinal grades sound like they are the same, but the requirements are quite different.
Pharmaceutical-grade products are manufactured using a set of standards called Good Manufacturing Practices, or GMP. There are different GMPs for different products, but pharmaceutical GMP is recognized as the highest, most stringent level of the GMP standards. It includes extensive requirements on manufacturing facilities, processes, documentation, training, testing, quality and operational procedures, distribution, packaging and labelling.
Pharmaceutical-grade products have been proven to be safe and effective through a rigorous clinical trial and regulatory process before they are approved by regulatory authorities and become available to consumers.
In contrast, medicinal-grade Cannabis products are made under a different set of standards to ensure safety and consistency, but they are not tested clinically. Medicinal-grade Cannabis can be sold at dispensaries, but cannot make health claims because they are not supported by data from clinical trials to demonstrate safety and efficacy. Since medicinal Cannabis is regulated at the state level, rather than federally, the level of quality and safety requirements vary widely.
Learn more about the different GMP requirements for pharmaceuticals, medicinal Cannabis, cosmetics, dietary supplements, and food and beverage products.
Current Cannabis-related products approved for therapeutic use
In the U.S., the Food and Drug Administration (FDA) has not approved cannabis for the treatment of any disease or condition. However, the FDA has approved one cannabis-derived and three cannabis-related drug products.
Epidiolex®, is an oral CBD formulation approved for the treatment of seizures associated with Lennox-Gastaut syndrome, Dravet syndrome and tuberous sclerosis complex. Epidiolex was approved in June 2018 and is the first FDA-approved drug that contains a purified drug substance derived from marijuana.
Marinol® and Syndros® are THC-related therapeutics approved by the FDA for the treatment of anorexia associated with weight loss in AIDS patients and to treat nausea and vomiting caused by chemotherapy. Marinol® and Syndros® contain dronabinol, a synthetic version of THC.
Cesamet® is another synthetic version of THC approved by the FDA to treat severe nausea and vomiting caused by chemotherapy. Cesamet® contains active ingredient, nabilone, a synthetic cannabinoid which has a chemical structure similar to THC.
Sativex® is a Cannabis -related drug not approved by the FDA in the U.S., but has been approved in Canada and several countries outside of the U.S. Sativex® is formulated from Cannabis extract and its main components are THC and CBD. Sativex® is an oromucosal spray approved in Canada for the symptomatic relief of multiple sclerosis-related spasticity (muscle stiffness/spasms).
Clinical trials are essential to prove medical benefits of a product
Well-controlled clinical trials to understand the true effectiveness and safety of the active compounds in Cannabis are needed to ensure safety for consumers. Clinical trials are conducted with compounds of known quality and potency. They are used to determine the optimal dose, and to discover any factors that affect dosing (e.g., preexisting health conditions, interactions with food or other drugs). Treatment outcomes are measured objectively and any safety signals are recorded. Once the benefits and risks are determined in a small group, the trials may be expanded to understand the compound’s effects on special populations, such as the elderly, the young, people with liver or kidney disease, or women who are pregnant or breastfeeding. All of this information is vital to developing safe prescribing instructions.
The same requirement should be expected for any medical use of Cannabis to ensure consumers know the potential dangers, limits, drug-to-drug interactions and proven efficacy.
The FDA notes they are aware of unapproved Cannabis and Cannabis-derived products being used to treat a number of medical conditions and cautions caregivers and patients that the use of unapproved Cannabis and Cannabis-derived products can have unpredictable and unintended consequences. FDA approved products have been carefully evaluated for safety, efficacy and quality and are continually monitored by the FDA after they are approved for the market.
InMed is the first and currently the only company to test cannabinol (CBN) in clinical trials as a potential therapeutic to treat disease. InMed’s INM-755 is a CBN cream under clinical development as a potential treatment for epidermolysis bullosa, a rare genetic skin disease. InMed is also conducting preclinical studies of drug candidate INM-088, an eyedrop CBN formulation being studied for its potential use as a glaucoma treatment for retinal ganglion cell protection and intraocular pressure reduction.
Safe use of Cannabis
As jurisdictions around the world begin to loosen their restrictions on the uses of Cannabis, regulation around safety remains a major concern. Without clinical trial evidence of Cannabis safety and efficacy, the onus is placed on physicians to determine dosing and potential side effects that may arise from prescribing medical Cannabis.
Medical organizations have asked for evidence to support health claims.
• Canadian Medical Association “While the CMA recognizes that some individuals suffering from terminal illness or chronic disease may obtain relief with Cannabis, there remains a need for clinical research, regulatory reviews and guidance for the use of Cannabis for medical purposes. Regulatory reviews are designed to protect patients and to provide critical information to physicians, such as clinical indications, dosages, and potential interactions with medications.”
• College of Family Physicians of Canada “Physicians cannot be expected to prescribe a drug without the safeguards in place as for other medications – solid evidence supporting the effectiveness and safety of the medication, and a clear set of indications, dosing guidelines and precautions.”
Concerns over illicit “synthetic cannabinoids”
There is a growing concern over the dangers of illicit human-made cannabinoids. These so-called ’synthetic cannabinoids’ are made from drying the Cannabis plant, then spraying it with additional mind-altering chemicals, creating potentially dangerous effects for users. According to the U.S. National Institute on Drug Abuse, synthetic cannabinoids are part of a group of drugs called new psychoactive substances (NPS), which are unregulated mind-altering substances intended to produce the same effects as illegal drugs. Synthetic cannabinoids exist under a number of brand names including K2, Spice, Joker, Black Mamba, Kush and Kronic.
Note that such illicit ‘synthetic cannabinoids’ are new chemical compounds that have different chemical structures from natural cannabinoids. These illicit ‘synthetic cannabinoids’ are also entirely distinct from the cannabinoids that are manufactured synthetically for pharmaceutical use, which are made to be bioidentical to natural cannabinoids as a way to ensure pharmaceutical-grade purity and consistency.
Resources
- FDA and Cannabis: Research and Drug Approval Process
- FDA Regulation of Cannabis and Cannabis-Derived Products, Including Cannabidiol (CBD)
- College of Family Physicians of Canada
- Canadian Medical Association – Advocating for a Public Health Approach to Cannabis
- Health Canada – Information for Health Care Professionals: Cannabis (marihuana, marijuana) and the cannabinoids
- PWC – Cannabis Report
- The Michael. G. DeGroote Centre for Medicinal Cannabis Research, McMaster University
- HealthLink BC – Medical Cannabis
- History of Cannabis as a medicine: a review
- The origins of cannabis smoking: Chemical residue evidence from the first millennium BCE in the Pamirs
- Oldest evidence of marijuana use discovered in 2500-year-old cemetery in peaks of western China
- History of cannabis as a medicine: a review
- Cannabinoid Receptors and the Endocannabinoid System: Signaling and Function in the Central Nervous System
- The discovery of the endocannabinoid system: Centuries in the making
- The Health Effects of Cannabis and Cannabinoids: The Current State of Evidence and Recommendations for Research
- National Institute on Drug Abuse – Synthetic Cannabinoids (K2/Spice) DrugFacts
Epidiolex® is a registered trademark of GW RESEARCH LIMITED
Marinol® is a registered trademark of ALKEM LABORATORIES LIMITED
Syndros® is a registered trademark of Insys Development Company, Inc.
Cesamet® is a registered trademark of Valeant Pharmaceuticals International
Sativex® is a registered trademark of GW Pharma Limited
Statements contained in this article have not been evaluated by the U.S. Food and Drug Administration (FDA) and are not intended to diagnose, treat or cure any disease. The studies mentioned in this article have not been conducted under formal human clinical trials or reviewed by a regulatory agency. The results of the studies referenced in this article have not been proven to diagnose or treat any disease. Always check with your healthcare practitioner before starting any new treatment. Readers are cautioned that the research contained in the article is not exhaustive. InMed Pharmaceuticals Inc. undertakes no obligation to update the information contained in the article, except as required by law.








